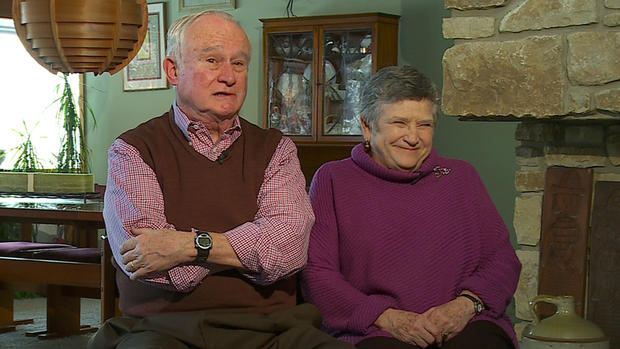Living With Memory Loss: A WCCO Special Report
MINNEAPOLIS (WCCO) -- At least half of us already know someone with Alzheimer's disease and in the next decade, twice as many Minnesotans will be diagnosed with it.
WCCO aired a special program Saturday night about the journey of one Twin Cities family.
Three years ago, retired physician Paul Quinn and his wife, Peg, invited photojournalist Tom Aviles and report Liz Collin to share their story. At 79 years old, a man who helped countless others heal is now facing a reality he always feared.
Part 1: Confronting A New Challenge
Paul Quinn has what doctors consider to be the earliest detectable stage of Alzheimer's, a disease that slowly destroys memory and thinking skills.
"Paul's goal and our goal as a family is to help people understand what the road is like," Paul's wife, Peg Quinn, said.
He and his family allowed our cameras to capture their daily lives with the diagnosis to see how one man who has helped countless others heal is facing a reality he always feared.
His smarts are envied and his story is exceptional. He's a doctor, an admiral and the center of a Twin Cities family.
We first met Peg and Paul Quinn in January.
"He was bright with a good sense of humor, very good looking," Peg recalled about the day they met.
"She had a good sense of humor," Paul recalled.
"What about the bright part?" Peg asked him.
"That speaks for itself," Paul joked. "Sometimes a little too much."
That sense of humor has been essential to their 50 years of marriage.
Paul grew up on the East Coast.
"He's from New Jersey," his oldest daughter, Mary McCallum, said. "He's Irish Catholic in a town of Italians."
His three daughters were witnesses to their dad's relentless work ethic and wide-ranging curiosity.
"He's always learning, curious about people, curious about trying new things," another daughter, Katie Mack, said. "He's one of the smartest people I've ever met."
Paul graduated from Notre Dame, went to medical school at the University of Michigan and became a family physician at Stillwater Medical Group.
At the same time, he rose through the Navy ranks to the highest position of admiral.
Paul's past is especially important when you get a glimpse of his future.
Paul first noticed memory problems as far back as five years ago.
"Everybody is experiencing it to a certain extent," Peg said. "The question is: Is what you're experiencing different than the average?"
Three years would pass before a diagnosis: Mild Cognitive Impairment, the early stages of Alzheimer's. Half the people with Mild Cognitive Impairment will develop Alzheimer's or another type of dementia within five years.
Dr. Michael Rosenbloom is the clinical director of HealthPartner's Center for Memory and Aging.
"Clearly the cognition is getting worse," Dr. Rosenbloom said. "However, his everyday function is relatively intact."
Rosenbloom has noticed Paul's disease hasn't developed as quickly as other patients.
"I think this has to do with his cognitive reserve," he said. "He's a very intelligent man. Sometimes with these patients you have this sense of denial, but Paul is very quick to say, 'You know what, my memory is impaired.'"
Paul's love for his field motivated him to do more in the fight. Since there's no medication to treat or cure his disease, he's part of a drug study to find one.
"I'm hopeful the trial I'm in will make a difference," Paul said. "If not for me, for other people."
Quinn family get-togethers are filled with the chaos of 12 grandkids.
"It's best to observe, not to participate," Paul joked. "It's safer."
Subtle reminders of Paul's struggle are felt by the whole family.
"Sometimes he kind of forgets who I am," one granddaughter told us.
"It kind of worries me, because I do know it will get worse over time," another said.
Two months after we first met Paul, he's having trouble remembering his grandkids' names.
"I'm in a situation where it's, 'Who is this? Who is that?' and then I'm scrambling and not coming up with anything," Paul said.
His honesty has to do with what he's already been through.
"My mother developed Alzheimer's," he said.
Several family members have shared the same fate.
Family history does play a role. Doctors have determined the risk for Alzheimer's increases if more than one person has had it in a family. But age is the biggest factor of all. After turning 65, the likelihood of developing the disease doubles ever five years.
Two years into his diagnosis, Paul still has a remarkable long-term memory. Doctors consider it a common misconception: While patients are losing their short-term memory, their long-term memory becomes more prominent.
"I have a lot better recollection of things of the past then the things of the now," Paul said.
Another daughter, Ann Vance, acknowledged it's been difficult for all of them.
"He came to my daughter's hockey games and he must have asked 10 times who they were playing, and mom looked at me and she said, 'This is my day, all day every day,'" Vance said.
It's why doctors often glean the most insight from a patient's caregiver to see how a person is progressing.
"The hardest part in the whole thing is seeing her," Katie Mack said about watching her mom go through it. "The nice part about Alzheimer's is he doesn't really know how bad he is."
The Quinns want to share their story to remind others they are not in this alone. It's a candid approach to their new reality that's clear in even the smallest of voices.
"I hope that it doesn't get really bad so he starts forgetting us," one granddaughter worried.
Doctors say being proactive about a diagnosis is important. Less than half of the people with Alzheimer's are diagnosed by their doctor. An honest diagnosis allows the person to plan for the future with their family. Some drugs may temporarily improve symptoms.
Part 2: Meet The Caregiver
Their routine, for the most part, has remained the same. Yet, there are subtle reminders of a steady change.
Paul still makes his breakfast each morning, but even a simple ritual can lead to confusion.
"What did I do with the sports section?" Paul asks again.
Paul is candid about his disease and its progression.
"I think I've continued to worsen," Paul said.
He was diagnosed with the earliest stages of Alzheimer's nearly three years ago, and after documenting his fight for the last year, we've noticed a turn.
He admitted he didn't remember my name when I asked him recently.
"At the moment, I don't," he said. "That's the kind of block you get."
"There is definitely a transition that is taking place," Peg added.
As a mother and grandmother, Peg has grown used to a caregiver role. Her main duty now is to her husband.
"I want to do everything in my power to make his life as enjoyable as possible," she said.
She's learned the importance of asking for help.
"When you're alone in a house together, it can be very depressing," Peg said. "It's good to get out and meet other people."
She meets with other Alzheimer's caregivers in the Stillwater area each month to hear how they can better cope with the daily struggles of the disease.
"I'm not very far along on this caregiver road," Peg said. "But, just to know there are other people that are in the same situation is really helpful."
Peg is also balancing her fears with Paul's freedom. He still drives on an almost daily basis.
"I've always had a good geographic feel for things," Paul said.
Experts believe caregivers shouldn't take a patient's independence from them too soon.
"The driving's been going well," Peg said. "I've been keeping my eyes out, and I think he's doing fine."
Perhaps the quality Peg best demonstrates is patience.
She never wants her husband to feel as if he shouldn't talk.
"I might hear it four or five times in 10 minutes, but it's the first time always for Paul," Peg said.
"If it's just a passing comment what difference does it make how many times it's asked," she added.
Finding a certain grace in Paul's struggle, she's determined to control what she can.
"If we can just focus on this good time that we still have left then that's the way to do it," Peg said.
Part 3: Coping With The Decline
He grew up an only child, but Paul has spent far more time as the patriarch of his own large family. For nearly a year and a half, we've watched them navigate the new waters Paul always feared, with a family history of Alzheimer's disease.
At Paul's most recent check-up, doctors take note of lasting cognitive skills. Still, there are signs of decline. He couldn't say what the date was when asked.
Katie Mack is Paul's youngest daughter.
"They seem like kind of trivial things, that who really cares," she said. "But when they add up throughout the day it's hard to watch because you realize that he has literally lost time."
Right now, what weighs heavy on the minds of Paul's family is the possibility of a quick slide in his condition.
"Then it won't be my dad anymore — that will be hard," Mack said. "Right now he's like a kinder, gentler version of my dad."
Mack keeps a journal to chart all of the changes, and even to record the silver linings along the way.
"My dad is more playful and sweet than he's ever been. It's weird," Katie reads. "Is it at all possible this Alzheimer's thing will provide gifts? I'm worried we're in the honeymoon stage, yet at this moment he's kinder and gentler than ever before."
In the last couple of years, his family has found it more difficult to have a two-way conversation with Paul. They focus instead on listening to keep him talking, even if it's a story they've already heard.
Paul's family worries more now about him driving than they did before. They've installed a new GPS tracking device on his car just in case.
Peg Quinn is Paul's wife.
"There is peace of mind knowing that it's there and that if we need t,o we should be able to find him," she said.
The kids have tried to divide duties as a way to help their mom pilot the progressive disease.
"I'm sure every adult with aging parents goes through those moments of, 'I really just want to see you as this strong, capable father. I don't really want to think about where you're going to live or how things are going to be for you in the next few years,'" Katie said.
Doctors think, for the most part, Paul's disease is progressing slowly, allowing a family more time to prepare for more difficult days ahead.
"Little bit scared and a little bit worried all the time because it's the unknown," Katie said. "How's this story going to end?"
------------------------------------------------------------------
The Alzheimer's Association staffs a 24/7 hotline for anyone to call with questions about the disease, 1-800-272-3900. The association also has lots of helpful resources on its website.
------------------------------------------------------------------
You can look back at all of our reporting with Paul Quinn here.